A patient recently came to my clinic holding his phone open to a dashboard of bright red dots from a wearable AI for sleep apnea. “My ring says I stopped breathing 42 times last night,” he told me. “Do I still need the sleep lab?” It’s a fair question, and the honest answer is more interesting than a yes or no.
Wearable AI for sleep apnea has moved fast. A 2025 systematic review in the Journal of Medical Systems found that rings, watches, and chest patches, paired with deep learning models, can now flag apnea events with surprising accuracy (Osa-Sanchez et al., J Med Syst, 2025). But “flag” is not “diagnose,” and “diagnose” is not “ready for surgery.” This article walks through what the 2025 evidence actually says, where consumer devices succeed, where they fail, and when you still need a sleep lab — or an ear, nose, and throat specialist.

How Wearable AI Actually Detects Sleep Apnea
Consumer devices do not measure airflow directly. They infer breathing events from surrogate signals: optical pulse measurements at the finger or wrist, blood oxygen saturation, heart rate variability, accelerometer-based body movement, and sometimes microphone-captured snoring audio. None of these are what a sleep lab uses to score an apnea.
The intelligence sits in the algorithm. Osa-Sanchez and colleagues reviewed 28 studies published between 2020 and 2024 and found that two families of deep learning models — convolutional neural networks and recurrent networks with long short-term memory — dominate the field, often boosted by transfer learning so a model trained on one population can be tuned to an individual wearer (Osa-Sanchez et al., J Med Syst, 2025). A separate 2025 Springer review by Huynh and colleagues, working with roughly 110,000 patient records from the French national sleep apnea registry, compared 39 machine learning models — but on electronic health record data, not wearable signals (Huynh et al., Machine Learning, 2025). The two research streams are related cousins, not the same tool.
Clinical perspective: When a patient tells me “the AI counted my apneas,” they usually mean a neural network made a probabilistic guess from a pulse waveform. That is not the same as a respiratory event scored by a sleep technologist against the American Academy of Sleep Medicine criteria.
How Accurate Is Wearable AI Compared to Polysomnography?
The most cited numbers come from a 2024 meta-analysis in the Journal of Medical Internet Research pooling 38 studies. Wearable AI achieved a pooled accuracy of 89.3%, sensitivity of 79.3%, and specificity of 94.7% (Abd-Alrazaq et al., J Med Internet Res, 2024).
Two details matter more than the headline.
First, specificity is high and sensitivity is lower. Translated clinically, the devices are good at telling a non-apneic user they are fine, but they miss roughly one in five true cases. A “negative” ring reading is less reassuring than it looks.
Second, the apnea event counts a wearable reports are not identical to the Apnea-Hypopnea Index from polysomnography. Sleep labs score events against standardized airflow and desaturation criteria reviewed by a technologist. Wearables estimate. The two numbers usually correlate; they are not interchangeable.
Where wearables systematically underperform:
- Central sleep apnea — wearables cannot distinguish loss of respiratory effort from true airway obstruction.
- Rapid eye movement sleep only apnea — events cluster in rapid eye movement sleep, which many consumer devices stage imperfectly.
- Positional apnea — supine-only events can be missed if the wearer rarely sleeps on their back during the recording window.

Smart Ring vs Smart Watch vs Patch: What’s the Difference in 2026?
Form factor changes what the sensor can see.
| Device | Main strength | Main weakness | Regulatory status (2026) |
|---|---|---|---|
| Smart ring (Oura, Ultrahuman) | Comfortable all-night wear, stable pulse signal at the finger | Blood oxygen calibration varies between units | Wellness tracker in most markets |
| Smart watch (Apple Watch, Samsung Galaxy Watch) | Ubiquitous, easy to deploy to millions | Wrist pulse signal is noisy with motion | Apple Watch sleep apnea notification is cleared by the FDA as a screening aid |
| Chest or forehead patch | Direct respiratory effort and position | Less comfortable, lower adherence | Some patches cleared at the home sleep apnea test level |
A ring and a watch are not a home sleep apnea test. A home sleep apnea test is a prescription device that records airflow, breathing effort, and oxygen saturation, and is interpreted by a sleep physician. Consumer wearables are adjacent to that category, not inside it.
When to Skip the Ring and See a Doctor
A wearable is a reasonable first filter for someone who wonders about their sleep. It is not the right starting point if any of the following are true:
- A bed partner has witnessed apneas or choking during sleep.
- You have resistant hypertension, atrial fibrillation, heart failure, or a recent stroke.
- Your Epworth Sleepiness Scale score is 10 or higher.
- You have morning headaches, refractory daytime fatigue, or cognitive complaints.
- Surgery is on the table — tonsillectomy, septoplasty, soft palate surgery (uvulopalatopharyngoplasty), or tongue base reduction.
In those situations a formal sleep study, and often an ear, nose, and throat evaluation, is the correct next step regardless of what the ring reports.
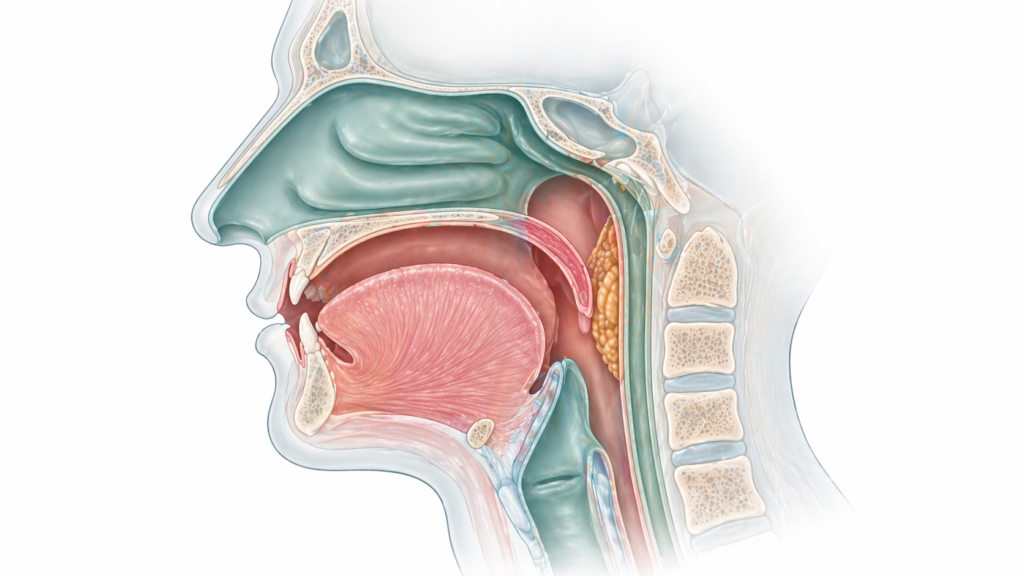
The ENT Surgeon’s View: What Wearables Cannot See
Here is the gap no consumer device closes: anatomy.
Wearable AI can count how many times you stopped breathing. It cannot tell you where the airway collapsed. In the surgical evaluation of obstructive sleep apnea, that “where” is the whole question.
When a patient is considering surgery, I still need to know:
- Tonsil size (graded on the Friedman classification) — large tonsils remain the single most common surgically correctable cause in younger adults.
- Tongue base and epiglottis behavior during sleep — assessed with drug-induced sleep endoscopy, not a ring.
- Nasal patency — septal deviation, inferior turbinate hypertrophy, and nasal valve collapse change how well a patient tolerates positive airway pressure therapy and how surgery should be sequenced.
- Palate and lateral pharyngeal wall tone — predicts response to soft palate surgery and expansion sphincter pharyngoplasty.
Clinical perspective: I think of the pathway as three gatekeepers. Wearables are the first — a broad, cheap, imperfect filter. Polysomnography is the second — it quantifies severity and confirms the diagnosis. The ear, nose, and throat surgeon is the third — the one who reads the anatomy and decides whether a scalpel belongs anywhere near this problem. Skipping any gate is how patients end up with expensive dashboards, correct diagnoses, and the wrong treatment.
Key Takeaways
- Wearable AI for sleep apnea in 2026 is a screening aid, not a diagnostic device.
- A 2024 meta-analysis found pooled sensitivity of 79.3%, meaning wearables miss roughly one in five true cases (Abd-Alrazaq et al., J Med Internet Res, 2024).
- The 2025 Journal of Medical Systems review identified rings, patches, and watches paired with deep learning as the most promising direction, especially when combined with transfer learning.
- Regulatory language matters: the Apple Watch sleep apnea notification is cleared for screening, not diagnosis.
- Surgery decisions require polysomnography plus an anatomic exam — no wearable can substitute for drug-induced sleep endoscopy or an ear, nose, and throat specialist’s evaluation of the upper airway.
FAQ
Can a smart ring diagnose sleep apnea? No. As of 2026, smart rings are regulated as wellness or screening aids, not diagnostic devices. A positive result from a ring is a reason to pursue a formal sleep study, not a replacement for one.
How accurate is wearable AI compared to polysomnography? A 2024 meta-analysis of 38 studies reported pooled accuracy of 89.3%, sensitivity of 79.3%, and specificity of 94.7%. Specificity is strong, but the sensitivity gap means roughly 20% of true cases are missed.
Should I skip the sleep lab if my Apple Watch says I’m fine? Not if you have witnessed apneas, daytime sleepiness, or cardiovascular risk. Wearables tend to miss central sleep apnea, rapid eye movement sleep only apnea, and positional apnea, so a negative wrist reading does not clearly rule out the disease.
When do I need to see an ear, nose, and throat specialist specifically? When a precise test or anatomical evaluation is being considered. Wearables cannot identify the site of airway obstruction — tonsils, tongue base, palate, or nose — and that information is what decides whether and how to operate.
Will AI replace polysomnography? Not for diagnosis in the current decade. AI is reshaping screening and is likely to absorb much of the “is this worth investigating” question, but polysomnography remains the reference standard for severity grading and treatment planning.
Joonpyo Hong, MD is a board-certified otolaryngologist practicing in Korea. This article reflects his clinical interpretation of published research and does not constitute individual medical advice.
References
- Osa-Sanchez A, Ramos-Martinez-de-Soria J, Mendez-Zorrilla A, Ruiz IO, Garcia-Zapirain B. Wearable Sensors and Artificial Intelligence for Sleep Apnea Detection: A Systematic Review. J Med Syst. 2025 May 19;49(1):66. DOI: 10.1007/s10916-025-02199-8
- Huynh TKC, Dabbs-Brown A, Jurek-Loughrey A, Mulhall J, Pham TD, Doan NP, et al. Obstructive sleep apnea prediction: a comprehensive review and comparative study. Machine Learning. 2026;115(2):Article 29. DOI: 10.1007/s10994-025-06937-4
- Abd-Alrazaq A, Aslam H, AlSaad R, et al. Detection of Sleep Apnea Using Wearable AI: Systematic Review and Meta-Analysis. J Med Internet Res. 2024;26:e58187. DOI: 10.2196/58187
This article is for educational purposes only and does not substitute for medical advice. If you have symptoms of sleep apnea, consult a qualified physician.